Post ROSC Care
A patient is brought to the ED following a cardiac arrest. ROSC is achieved 1 minute after arrival to the ED. What treatments should the ED physician provide to allow the best outcomes?
A patient is brought to the ED following a cardiac arrest. ROSC is achieved 1 minute after arrival to the ED. What treatments should the ED physician provide to allow the best outcomes?
Its 3am in the ED and you need to call a consult. What strategies can you use to get great care for your patients and be a good colleague?
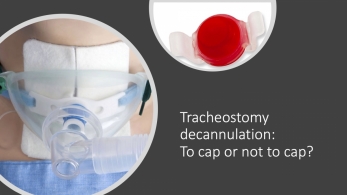
A 49-year-old woman was intubated for acute hypoxemic respiratory failure secondary to pneumonia, which was complicated by empyema. She failed extubation and ultimately required tracheostomy for prolonged mechanical ventilation. After transfer to the intermediate care unit, she was successfully weaned from the ventilator for over 24 hours. She tolerated prolonged deflation of her tracheostomy cuff and swallowed water without aspiration. She underwent a tracheostomy tube occlusion test and there was no obstruction to air flow with a size 7 fenestrated tracheostomy tube in place. She is requiring suctioning once every 12 hours. You are assessing her readiness for tracheostomy decannulation and are considering the utility of a capping trial.
It’s a familiar call ahead to the ED - an adult patient who is febrile, hypotensive, with suspicion towards infection. While setting up the room, the patient’s bedside nursing team asks if you’d like them to get saline or lactated Ringer’s (LR) ready for resuscitation. You wonder if there’s any new evidence examining the use of saline versus balanced crystalloids in the emergency department.
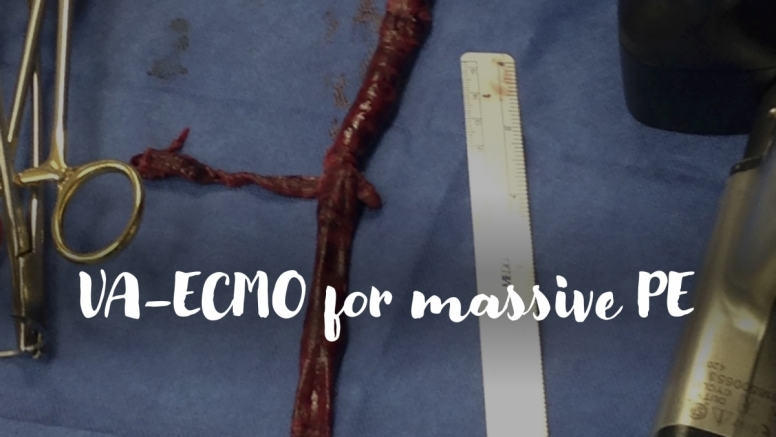
A 60-year-old man presents to the ED after an episode of syncope. He is initially hemodynamically stable and undergoes CT demonstrating saddle pulmonary embolism. He returns from radiology with tachycardia and hypotension refractory to fluids and requiring vasopressor support. Bedside echo reveals RV dilation and severely reduced RV systolic dysfunction with septal flattening consistent with RV pressure overload. As you start systemic anticoagulation with heparin, you consider the indications for thrombolysis, surgical embolectomy and VA-ECMO.
EMS calls ahead with reports of an adult patient in respiratory distress. They are concerned the patient will need to be intubated on arrival. Recognizing the name, you pull up a previous chart and review the patient’s history. You realize this is their 10th presentation this year and on reviewing their most recent oncology note you note their oncologist has recommended they consider hospice due to end stage malignancy without further treatment options. The patient arrives, is in distress, and does not have capacity but can be temporized by NIPPV while decision making occurs. Their power of attorney comes to the hospital soon after but states they never got around to establishing an advanced directive. How should you approach this conversation?

Several drugs have been investigated in patients with ARDS, including epoprostenol, nitric oxide, statins, and methylprednisolone, but have not improved survival. Meduri et al. performed an RCT demonstrating that methylprednisolone was associated with a reduction in lung injury score and duration of mechanical ventilation. While not powered to evaluate mortality, this trial raised interest in the use of corticosteroid to mitigate inflammatory lung injury. The 2017 Guidelines from the Society of Critical Care Medicine (SCCM) and the European Society of Intensive Care Medicine (ESICM) recommend steroids for treatment of ARDS based on a meta-analysis of nine randomized controlled trials demonstrating reduction in markers of inflammation and duration of mechanical ventilation, although many of the trials had a small sample size and some were performed without lung protective ventilation. In March 2020, Villar et al. published the largest randomized control trial of corticosteroid therapy for moderate to severe ARDS investigating the impact of dexamethasone on survival and duration of mechanical ventilation.
You admitted a 72 year old male to the ICU for septic shock from community acquired pneumonia. He required intubation and mechanical ventilation for failure to improve oxygenation with NIPPV and encephalopathy. He received broad spectrum antibiotics and a 30 cc/kg crystalloid bolus. His MAP was persistently in the 50s despite adequate fluid resuscitation and based on your exam he does not appear hypovolemic. Norepinephrine is started and despite adequate MAP he is oliguric. His only medical history is he was a previous smoker with COPD, HTN, HLD but normal renal function with a Cr of 0.8 two months prior. His Cr on admission is 2.2 and a foley is placed and his UA shows granular casts. He is not acidotic and his electrolytes are normal.
You are concerned this patient is heading towards renal replacement therapy. He is adequately fluid resuscitated and has a MAP above 65 on a vasopressor but is still not making urine and has signs of ATN on urinalysis. Renal replacement therapy is an invasive procedure and has associated risks. If a patient has a chance to have renal recovery with a more conservative approach then this should be considered. You wonder if there is a diagnostic test which can be used to assess the potential for renal recovery.

A 34-year-old woman at 32 weeks gestation presents to the emergency department with cough, dyspnea and hypoxemia. She rapidly progresses to severe ARDS despite lung protective ventilation, paralysis and inhaled epoprostenol. P/F ratio is 99 mm Hg. Is prone positioning safe to perform in pregnant patients with severe ARDS? If so, are modifications necessary to offload the abdomen and monitor the fetus? A recently published review in Obstetrics and Gynecology discusses this important topic.
A 56 year old male comes to the ED via EMS after noting progressive dyspnea and fever. In the field, the EMS team notes the patient is hypoxic with an SPO2 of 85%. Despite the low oxygen saturation, he is only using minimal accessory muscles and he is alert and oriented. His chest X-ray shows a right lobar pneumonia and he is requiring 6LNC oxygen to maintain a saturation greater than 90%. You know there is significant guideline evidence to support the use of non-invasive positive pressure ventilation (NIPPV) for COPD and CHF exacerbations, but what about patients with other causes of hypoxia such as pneumonia?
Copyright © 2024,
Designed by Zymphonies
